Prof. Komi de Souza is an Associate Professor of Parasitology at the Noguchi Memorial Institute for Medical Research, University of Ghana, where he leads the Neglected Tropical Diseases Group and serves as Head of the Department of Clinical Pathology. His research focuses on lymphatic filariasis and other NTDs, advancing diagnostics and elimination strategies. Through international collaborations, mentoring young scientists, and projects such as SENTINEL and multi‑country evaluations of novel diagnostics, he is strengthening Africa’s capacity in parasitology and public health while demonstrating how Ghanaian research can drive global impact.

Prof. Komi de Souza , Associate Professor of Parasitology at the Noguchi Memorial Institute for Medical Research (NMIMR), University of Ghana
In a spotlight interview, we engaged with Professor de Souza, whose impactful research on neglected tropical diseases is connecting Ghana to global health efforts.
Priscilla Kissi: What inspired you to choose science as a career and neglected tropical diseases (NTDs) as your research domain?
Prof. de Souza: I’ve always loved science and wanted to become a cardio-thoracic surgeon or a paediatrician. However, medical school didn’t choose me, and I found my way to NMIMR for an internship. That was where I was introduced to my first research on Buruli ulcer, and NTD. Research suited me and allowed me to travel, engage with communities, and make an impact. At the end I am glad medical school did not work.

From classroom curiosity to global health leadership, Prof. de Souza and his team stand united on World NTD Day, turning research into real impact for communities in Ghana.
Priscilla Kissi: How would you explain NTDs in everyday language?
Prof. de Souza: They are diseases that disproportionately affect the poor. A wealthy person can get them too, but they can afford quick treatment. For the poor, these diseases linger, causing long-term suffering, stigma, and exclusion. That’s why they’re called neglected they lacked the funding and attention given to diseases like malaria, HIV and TB.
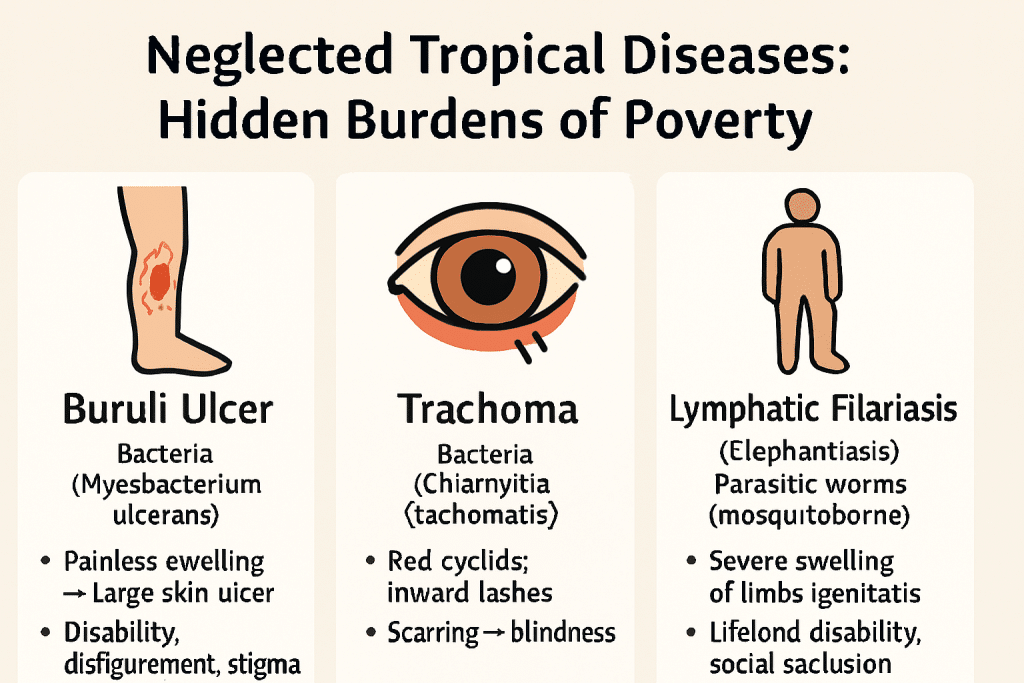
Visual explanation of Neglected Tropical Diseases (NTDs)
Priscilla Kissi: Looking back to when you first chose to work in NTD research, how has the field evolved, especially in terms of diagnostic advancements and support for affected individuals?
Prof. de Souza: Tremendously. In the past, doctors had to rely mainly on what they could see, symptoms of the diseases and simple microscopy to check for parasites. These methods often missed early infections and required highly trained specialists. Later, molecular tools such as PCR began to help us detect very small amounts of parasite DNA, but they were expensive and not widely available. Today, things have changed dramatically. We now have rapid diagnostic tests that give results in minutes, advanced molecular techniques that are more precise, and a stronger focus on patient-centred care. Thus, we don’t just treat the infection, but also address the stigma, disability, and mental health challenges that come with NTDs.

NTD Team empowering communities with rapid diagnostic tests and patient‑centred care at a community outreach.
Priscilla Kissi: Leading a team comes with big challenges. As Head of the NTD Group, what are the biggest challenges in eliminating lymphatic filariasis and other neglected tropical diseases?
Prof. de Souza: Funding is a critical concern, given the change in the current funding and geopolitical landscapes. As such working towards domestic resource mobilization is important for the sustainability of the NTD elimination efforts. Another challenge is the detection of the few remaining cases, following successful disease elimination campaigns. If missed, these missed cases can be reservoirs of infection and can reintroduce the disease to the communities. Communities also grow tired of mass drug administration after many years, especially when the disease is no longer visible. There is also the need to provide care and psychosocial support to patients affected with the disabling nature of some NTDs.

Essential care items for those living with NTDs provided by NMIMR at an NTD outreach at Ga Municipal Hospital (Amasaman)
Priscilla Kissi: Your current work is shaping the future of public health. Can you tell us about your current projects, like the facility-based surveillance study?
Prof. de Souza: Our Facility-based surveillance study aims to integrate the diagnosis of lymphatic filariasis with malaria, since both are transmitted by the same vectors in Ghana. This way, the diagnosis, identification and reporting of the few remaining cases can be integrated in the health system, rather than relying on limited surveillance campaigns. We are also developing new rapid diagnostic tests to improve the diagnosis of Schistosomiasis.
Priscilla Kissi: When people hear about neglected tropical diseases, it can sound very complicated or out of reach. But for families living with them, the impact is very real and personal. Can you share an example of how your work has touched the lives of families in Ghana?
Prof. de Souza: We have seen parents with lymphatic filariasis unable to work or send children to school. Once adequately managed or treated, they regain stability and can care for their families again. That’s the real impact, restoring dignity and livelihood.

Prof. de Souza and his team touching lives in Ghana through care, and gifts that support families affected by NTDs.
Priscilla Kissi: Was there an ‘aha’ moment in your studies or career when you realized good diagnostics could truly save lives?
Prof. de Souza. Yes, during my WHO/TDR fellowship at FIND (the Foundation for Innovative New Diagnostics) in Geneva. I learnt the real importance of diagnosis and the fact that without diagnosis, treatment was blind. For any disease, adequate diagnosis is the start of the healing process. Having worked on diseases like visceral leishmaniasis where the treatment was very toxic, it was absolutely important to confirm diagnosis before putting patients on the drugs. Make diagnostics available where they are needed was also critical in ensuring access. Working at FIND made me realise how critical diagnostics are, and it shaped my career to focus on developing better ways to detect diseases and save lives.
Priscilla Kissi: Looking back often shows what truly mattered, which achievement makes you most proud, and why?
Prof. de Souza: I am not particularly proud of any single achievement. But I am grateful for the opportunity to contribute in meaningful ways. My life’s work has focused on improving the diagnosis and advancing the elimination of NTDs. If my efforts have in any way strengthened systems, supported communities, or moved us closer to controlling and eliminating these diseases, then that for me is achievement enough.
Priscilla Kissi: Local research can open doors to global collaboration. How has your work at NMIMR connected Ghana to global health efforts? Do you feel global partners are fully engaged, or expecting Africans to carry more of the effort funds because this is considered a tropical disease and they are providing the research?
Prof. de Souza: Many of our studies at the NMIMR have contributed to shaping international health policies. In other words, the research we do here in Ghana doesn’t stay local, it helps guide how countries around the world fight NTDs. Through partnerships, NMIMR shares knowledge and learns from global colleagues, ensuring that African research is recognised and contributes meaningfully to worldwide solutions.

Prof. de Souza at a meeting at the WHO, in Geneva Switzerland.
Priscilla Kissi: Beyond lymphatic filariasis, which neglected diseases deserve more attention?
Prof. de Souza: No NTD deserves attention more than others. They are all equally important. Even if only one person is affected, the impact can be devastating for that individual and their family. That’s why no NTD should be seen as less important than another.
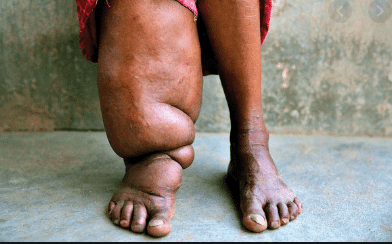
A Picture of Lymphatic Filariasis (LF)
Priscilla Kissi: Strong health systems start with strong diagnostics. What steps can Ghana and other African countries take to improve testing and diagnosis of NTDs?
Prof. de Souza: African countries need to invest in better diagnostic capabilities and train more skilled health workers. It’s also important to make sure medical supplies reach where they’re needed and to include diagnostic tests in everyday healthcare services, and not just at specialized centres. Supporting local production of tests will make them more affordable and accessible. Finally, using digital systems to report and track cases can help health officials respond faster and more effectively.

NMIMR health worker educates locals on NTDs to boost early diagnosis and testing.
Priscilla Kissi: Finally, every journey inspires the next generation, what advice would you give to young students who want to study science and NTDs?
Prof. de Souza: Don’t go into science for money go because you’re passionate and curious about it. Be persistent, define your purpose, and find mentors who can guide you. Even the most intelligent person needs someone to open doors for them.

Prof. de Souza inspiring the next generation of scientists through educational community outreach, reminding young minds that science is driven by passion, curiosity, and mentorship, not money.
Priscilla Kissi: Science is a passion. You must be curious and persistent. Thank you, Professor, for sharing your insights and inspiring the next generation.
Prof. de Souza: You’re welcome.

